8.3.9.4. Biological Agents: Vector- and Waterborne Diseases
8.3.9.4.1. Vector-borne diseases
Changing climate conditions may lead to the northward spread of vector-borne
infectious diseases and potentially enhanced transmission dynamics as a result
of warmer ambient temperatures.
Vector-borne diseases (primarily carried by arthropod or small mammal "vectors")
and waterborne diarrheal diseases represent a large proportion of infectious
diseases, which are the world's leading cause of fatalities. Projected changes
in climate almost certainly would make conditions less suitable for the transmission
of several vector-borne diseases (e.g., plague and some forms of encephalomyelitis)
in much of their current North American range. Other diseases (e.g., Saint Louis
encephalitis and western equine encephalomyelitis) might extend their range
northward or exhibit more frequent outbreaks. The crucial factor is the availability
of appropriate habitats for vectors and (in the case of zoonotic diseases) vertebrate
"maintenance" hosts. Although projected changes in climate might provide opportunities
for diseases to extend their range, the North American health infrastructure
may prevent a large increase in disease cases; providing this protection, however,
could increase the demands on and costs of the current public health system.
The transmission of many infectious diseases is affected by climatic factors.
Infective agents and their vector organisms are sensitive to factors such as
temperature, surface water, humidity, wind, soil moisture, and changes in forest
distribution (IPCC 1996, WG II, Chapter 18).
Malaria: Climatic factors, which increase the inoculation rate of Plasmodium
pathogens and the breeding activity of Anopheles mosquitoes, are considered
the most important factors contributing to epidemic outbreaks of malaria in
nonendemic areas. A temperature relationship for sporadic autochthonous malaria
transmission in the temperate United States has been observed in New York and
New Jersey during the 1990s (Layton et al., 1995; Zucker, 1996). Common to these
two outbreaks was exceptionally hot and humid weather, which reduced the development
time of malaria sporozoites enough to render these northern anopheline mosquitoes
infectious. Such temperature sensitivity of parasite development also has been
observed in the laboratory (Noden et al., 1995).
Martens et al. (1995) estimated that an increase in global mean temperature
of several degrees by the year 2100 would increase the vectorial capacity of
mosquito populations 100-fold in temperate countries. In these countries, however,
continued and increased application of control measures-such as disease surveillance
and prompt treatment of cases-probably would counteract any increase in vectorial
capacity. Similarly, Duncan (1996) showed that projected increases in mean daily
temperatures may allow for the development of malaria in Toronto. It was not
suggested, however, that climate alone would permit the spread of malaria because
many other factors must be considered.
Malaria once prevailed throughout the American colonies and southern Canada
(Russell, 1968; Bruce-Chwatt, 1988). By the middle of the 19th century, malaria
extended as far north as 50°N latitude. In Canada, malaria disappeared at the
end of the 19th century (Bruce-Chwatt, 1988; Haworth, 1988). Serious malaria
control measures were first undertaken in the southern United States in 1912
(Bruce-Chwatt, 1988). By 1930, malaria had disappeared from the northern and
western United States and generally caused fewer than 25 deaths per 100,000
people in the South (Meade et al., 1988). In 1970, the World Health Organization
Expert Advisory Panel on Malaria recommended that the United States be included
in the WHO official register of areas where malaria had been eradicated. The
history of malaria in North America reinforces the suggestion that although
increased temperatures may lead to conditions suitable for the reintroduction
of malaria to North America, socioeconomic factors such as public health facilities
will play a large role in determining the existence or extent of such infections.
Arboviruses: Dengue fever and dengue hemorrhagic fever (DHF) periodically
have occurred in Texas, following outbreaks in Mexico, during the past two decades
(Gubler and Trent, 1994; PAHO, 1994). Because of the sensitivity of dengue to
climate, especially ambient temperature, it has been suggested that this disease
may increase in the United States if a sustained warming trend occurs. However,
due to high living standards, this disease is not likely to increase in incidence
or geographic distribution in the United States, even if there is a sustained
warming trend. Dengue viruses occur predominantly in the tropics, between 30°N
and 20°S latitude (Trent et al., 1983); freezing kills the eggs, larvae, and
adults of Aedis aegypte, the most important vector (Chandler, 1945; Shope, 1991).
It should be noted, however, that the eggs of Ac. Alhopictus, also a vector,
are not killed by freezing.
Jetten and Focks (1997) analyzed the impact of a 2°C and a 4°C temperature
rise on the epidemic potential for dengue, including the impacts for cities
in temperate areas (Figure 8-11). Their analysis shows
that areas adjacent in latitude or elevation to current endemic zones may become
more receptive to viral introductions and enhanced transmission. Furthermore,
their study shows that the proportion of the year when transmission can occur
in North America could significantly increase under warming scenarios.
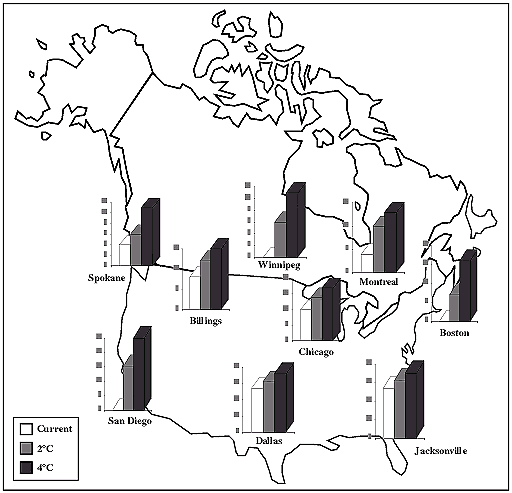 |
| Figure 8-11: Weeks of potential dengue transmission under current
temperature and 2°C and 4°C warming (adapted from Focks et al., 1995; Jetten
and Focks, 1997). Presence of dengue virus, mosquito vector, and exposed
human populations are required for disease transmission. |
(continues on next page...)
|